Vol 126: Gift of a stranger
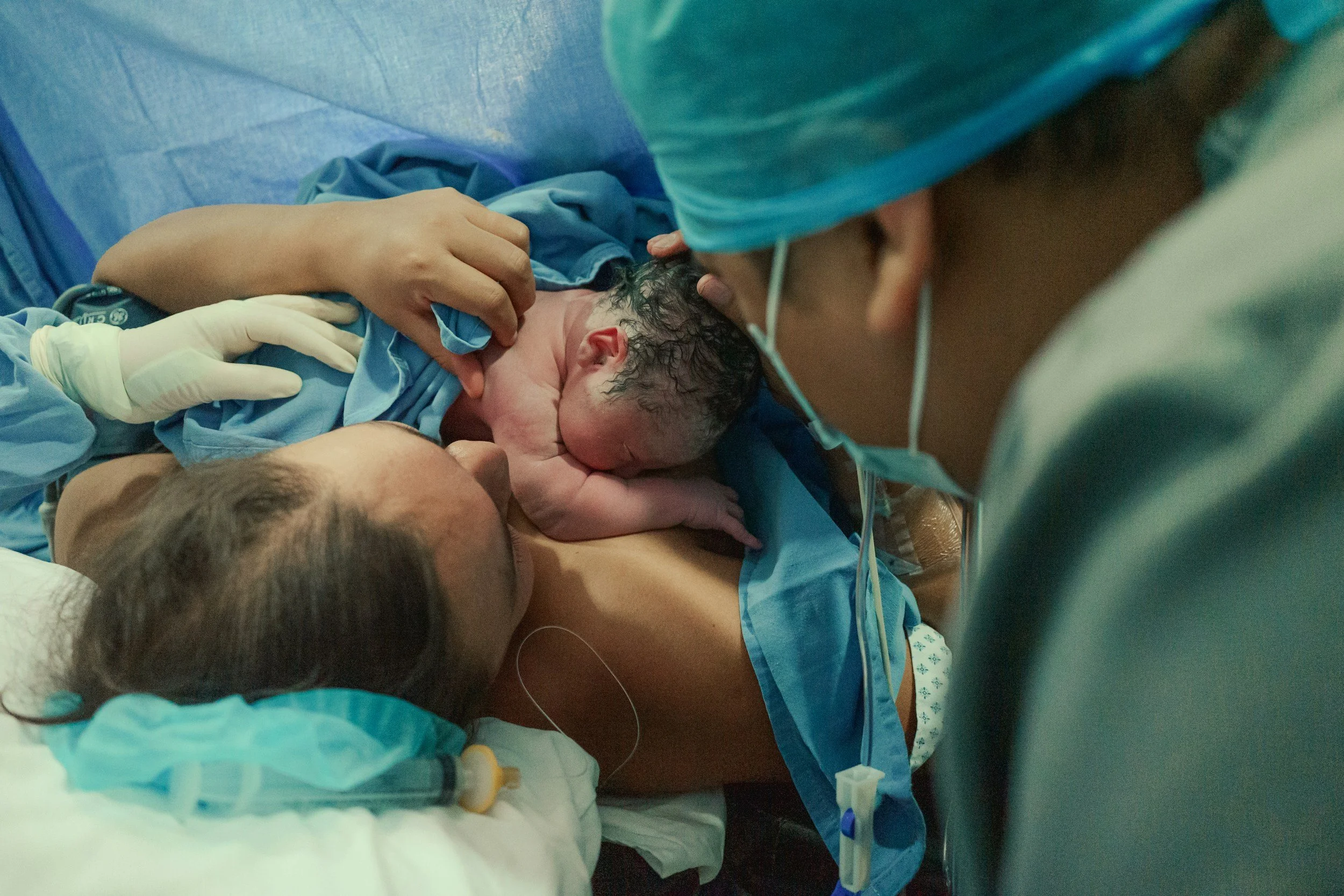
Imagine it’s 3 a.m. Your wife goes into labor. There’s excitement, nervous laughter, the hurried drive through quiet streets. By the time you reach the hospital, you’re thinking about finally holding your baby and whispering the name you agonized over. You think about first cries and ultimately about the moment your life will change forever. But instead, your wife’s doctor pulls you aside.
There are complications. A severe postpartum hemorrhage. It’s one of the most common and dangerous emergencies in obstetrics; unpredictable, fast-moving, and unforgiving. The blood loss is significant and blood is needed immediately. But that sentence is quickly followed by another no family should ever have to hear; there isn’t enough blood available right now.
What should have been a medical emergency managed with precision the way we see it in so many gripping TV shows becomes something far more fragile and fraught with fear. Frantic phone calls are made to sleeping family, friends and neighbors, begging them to donate blood and to call everyone they can. They reach out to their network, they post the cry for blood on social media, and soon strangers are asked to leave their beds and rush to the hospital. You pace the floor, hands sweating, heart caught between thumping and breaking, hoping someone will arrive in time and that someone not only has the right blood type but is able to meet all donation requirements.
All while a mother and child wait.
This is not a hypothetical scenario. It’s one I have seen echoed repeatedly through my patients’ stories at both Doctors Hospital and Princess Margaret Hospital in Nassau and undoubtedly at Rand Memorial in Grand Bahama. At some point, it may more than likely occur at the new Eleuthera Wellness Hospital. The names and scenarios change, the diagnoses vary but the fear does not.
Chronic and recurrent blood shortages have quietly become part of an insidious back story of our healthcare landscape. We treat them as unfortunate but inevitable, responding the same way each time, with urgent appeals and last-minute heroics. But improvisation is not a system. And hope is not a strategy.
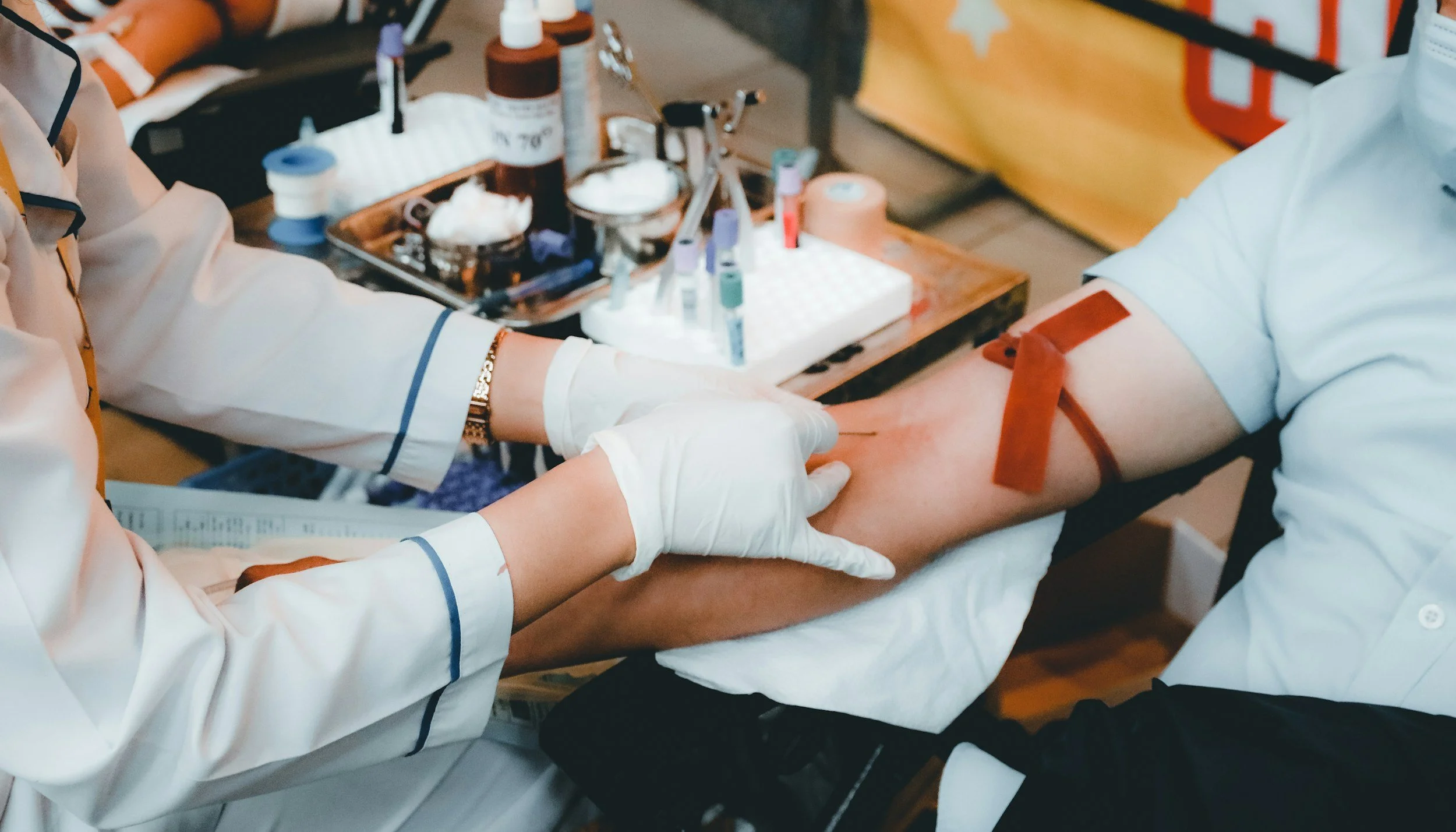
Blood donation is governed by necessary standards. Donors must meet age, weight, and hemoglobin thresholds. Certain medical conditions, medications, recent illnesses, recent tattoo or travel histories can lead to temporary or permanent deferral. Even well-intentioned volunteers may arrive only to be told they cannot donate. These safeguards protect recipients, but they also expose the weakness of relying on chance when lives are at stake. But there is a better option.
I believe this cycle can be broken. And more importantly, it must be. The solution isn’t more emergency appeals; it’s a fundamental reimagining of how we approach blood donation in The Bahamas. I’m advocating for the creation of a national blood donor registry, a proactive, organized, ready-to-deploy system designed not for crisis response, but for crisis prevention. Here is how it would work.
First, we identify and register 50 eligible donors for each blood type (A, B, AB, O) inclusive of all Rh-positive and Rh-negative subtypes. We can do this through invitation or public notice for volunteers. These individuals would be screened, blood-typed, and entered into a secure national database with full confidentiality. Their eligibility status would be updated regularly, ensuring that when blood is needed, hospitals are not searching blindly but activating a readily available, reliable pool.
Second, donors would receive an official blood donor card that serves as a symbol not only of willing civic responsibility but of partnership. Participating hospitals and private clinics would agree to recognize this card with tangible benefits: reduced, deferred, or waived co-payments when appropriate, expedited services and appointments, and formal acknowledgment of the donor’s contribution to national health.
Importantly, these incentives are not a financial risk to participating institutions or businesses; they’re a strategic investment. Anyone eligible to donate blood is, by definition, likely to be relatively healthy. Hospitals and private clinics that extend privileges to donors are therefore not inviting excessive utilization or financial strain, but rather engaging a population that already demonstrates preventive health behaviors. At the same time, businesses that offer modest discounts benefit from increased customer loyalty, positive public perception, and consistent patronage from a clearly defined and socially responsible group.
Third, this effort would extend beyond medicine alone. Grocery stores, gas stations, clothing stores, gyms, pharmacies, shopping centers, restaurants, and other local businesses could participate by offering modest discounts or incentives to registered donors. Not as payment, but as recognition. A public signal that donating blood is not an invisible act, but a valued one.
Health insurers could also offer modest incentives to registered blood donors like wellness credits or reduced deductibles. Life insurers, too, would have a clear incentive to participate as every life saved means sustaining coverage, not settling a loss.
The benefits extend even further. A national blood donor registry would not only save lives in moments of crisis; it would quietly but ideally encourage a healthier population overall. In a country ranked among the highest globally for obesity and non-communicable diseases, eligibility itself becomes motivation. Weight loss, improved blood glucose control, better blood pressure management - each becomes a step toward qualifying for a coveted donor card and the privileges that accompany it. Health, in this model, is no longer abstract; it is tangible, recognized, and rewarded.
Most importantly, this registry would replace panic with preparedness. No more frantic middle-of-the-night calls. No more uncertainty about blood type compatibility or eligibility. No more families wondering whether help will arrive in time. As physicians, we are trained to anticipate complications and prepare for them. As a society, it is imperative we do the same.
There are countless moments in any hospital week when the need for blood arises, but we continue to treat each instance as though it were extraordinary. Imagine if every time a nurse needed a bandage, or a doctor required a splint to stabilize a broken bone, they were forced to scramble, making calls, appealing to strangers by posting on social media, all while a patient waited in agony with a limb left unsupported. It would be unthinkable. Yet, the collection of blood, which is the most essential element of care beyond the human touch itself, is still treated as a sideline to the provision of care.
In moments of crisis, survival may not always be dictated by medicine alone, but on the quiet generous gift of a stranger. While The Bahamas has a smaller population, fewer trauma cases, and far fewer mass-casualty events than larger countries, the ongoing demand for blood remains high because it’s driven by obstetric emergencies, surgical care, chronic anemia, sickle cell disease and a disproportionately large dialysis population in a country with limited access to kidney transplantation.
Donated blood expires within weeks and despite modern medicine, despite innovation, despite machines capable of replacing hearts and filtering kidneys, blood cannot be manufactured. There is no artificial substitute. No laboratory-grown equivalent. Every unit still requires one person to willingly give a part of themselves so that another might live.
No mother should bleed while a system scrambles. No child’s survival should depend on chance. And no family should learn, in their most vulnerable moment, that the lifeline they need simply isn’t there.
The Bahamas has always been a nation of neighbors helping neighbors. A national blood donor registry simply gives that impulse the structure it needs to save lives consistently, predictably, and sustainably. This is not an unsolvable problem. It is an organizational one. And with compassion, coordination, and common sense, it is entirely possible to achieve.
This is The KDK Report